|
Overview
The most common arch problem is the flat foot. This sometimes starts in childhood or may gradually develop in adulthood. In most cases the flat foot is related to a tight calf. The tightness of the calf forces the foot to overpronate (the inside of the foot rolls inwards) and the arch to break down and collapse. The arch collapse leads to abnormal stress on the plantar fascia leading to heel pain, as well as to the main medial tendon (the posterior tibial tendon), leading to tendonitis and even tears of the tendon. The other common symptom in severe flat feet is pain on the outside of the foot as well as calf and Achilles symptoms. Causes There is a lack of normal arch development, probably due to inherent ligamentous laxity. Around 20% of adults have Pes planus. The majority have a flexible flat foot and no symptoms. However, if there is also heel cord contracture, there may be symptoms (see 'Contributing factors', below). Loss of support for the arch. Dysfunction of the tibialis posterior tendon, a common and important cause. Tear of the spring ligament (rare). Tibialis anterior rupture (rare). A neuropathic foot, e.g from diabetes, polio, or other neuropathies. Degenerative changes in foot and ankle joints. Inflammatory arthropathy, eg rheumatoid arthritis. Osteoarthritis. Fractures. Bony abnormalities, eg tarsal coalition. Symptoms Knee/Hip/Back Pain - When the arch collapses in the foot, it triggers a series of compensations up the joint chain, leading to increased stress on the knee, pelvis and low back. Plantar fasciitis - This condition is characterized by heel pain, especially with the first few steps you take. The plantar fascia stretches as the arch falls, putting stress on the heel. Bunions - If you see a bony bump developing at the base of your big toe, you are likely developing a bunion. It may be swollen, red or painful when it rubs against your shoe. A flattened arch spreads the forefoot and causes the big toe to deviate toward the second toe. Shin splints - This term generally refers to pain anywhere along the shinbone. It is typically due to overuse and is aggravated after exercise and activity. Diagnosis Most children and adults with flatfeet do not need to see a physician for diagnosis or treatment. However, it is a good idea to see a doctor if the feet tire easily or are painful after standing, it is difficult to move the foot around or stand on the toes, the foot aches, especially in the heel or arch, and there is swelling on the inner side of the foot, the pain interferes with activity or the person has been diagnosed with rheumatoid arthritis. Most flatfeet are diagnosed during physical examination. During the exam, the foot may be wetted and the patient asked to stand on a piece of paper. An outline of the entire foot will indicate a flattened arch. Also, when looking at the feet from behind, the ankle and heel may appear to lean inward (pronation). The patient may be asked to walk so the doctor can see how much the arch flattens during walking. The doctor may also examine the patient's shoes for signs of uneven wear, ask questions about a family history of flatfeet, and inquire about known neurological or muscular diseases. Imaging tests may be used to help in the diagnosis. If there is pain or the arch does not appear when the foot is flexed, x-rays are taken to determine the cause. If tarsal coalition is suspected, computed tomography (CT scan) may be performed, and if an injury to the tendons is suspected, magnetic resonance imaging (MRI scan) may be performed. pes planus radiology Non Surgical Treatment Switch activities for a little while. If you?re a super athlete, you don?t want to hear that you need to take a break, but there?s no way around it. You need to lay off the high impact sports like basketball, tennis and running. Don?t panic-there?s no shortage of alternatives. Find a high school track that?s open to the public and try going for a run. Many athletic programs use spongy synthetic materials to pave tracks instead of concrete. This is much easier on all the joints and tendons, not only in your feet but your legs and ankles. You can also try running on dirt trails or stable grassy areas. Take up swimming for a little while. This is actually an ideal activity for your arches. The buoyancy of water takes weight off our feet, but still allows for aerobic activity. Many gyms and activity centers also offer various water sport classes. In no time flat, you?ll be on your way to healthier feet. Surgical Treatment  This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Overview
 Heel pain is a common foot condition. It's usually felt as an intense pain when using the affected heel. Heel pain usually builds up gradually and gets worse over time. The pain is often severe and occurs when you place weight on the heel. In most cases, only one heel is affected, although estimates suggest that around a third of people have pain in both heels. The pain is usually worse first thing in the morning, or when you first take a step after a period of inactivity. Walking usually improves the pain, but it often gets worse again after walking or standing for a long time. Some people may limp or develop an abnormal walking style as they try to avoid placing weight on the affected heel. Causes Heel pain can have many causes. If your heel hurts, see your primary care doctor or orthopaedic foot and ankle specialist right away to determine why and get treatment. Tell him or her exactly where you have pain and how long you've had it. Your doctor will examine your heel, looking and feeling for signs of tenderness and swelling. You may be asked to walk, stand on one foot or do other physical tests that help your doctor pinpoint the cause of your sore heel. Conditions that cause heel pain generally fall into two main categories: pain beneath the heel and pain behind the heel. Symptoms The symptoms of plantar fasciitis are pain on the bottom of the heel, pain in the arch of the foot, pain that is usually worse upon arising, pain that increases over a period of months. People with plantar fasciitis often describe the pain as worse when they get up in the morning or after they?ve been sitting for long periods of time. After a few minutes of walking the pain decreases, because walking stretches the fascia. For some people the pain subsides but returns after spending long periods of time on their feet. Diagnosis A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans. Non Surgical Treatment Initial treatment consists of rest, use of heel cushions to elevate the heel (and take tension off the Achilles), stretching and applying ice to the area. You can ice and stretch the area simultaneously by filling a bucket with ice and cold water and placing the foot flexed with the toes upward so that the Achilles tendon region is bathed in the cold water for 10 to 15 minutes twice a day. The Achilles region can also become inflamed around the tendon, called paratendinosis. This condition can be treated with the ice bucket stretching, rest and physical therapy. Another area that is commonly subjected to problems is the attachment of the Achilles near or on the heel bone. The heel (calcaneus) itself can have an irregular shape to it, causing irritation to the Achilles as it twists over the region and inflames the bursa, a naturally occurring cushion. Shoes can often aggravate this condition. Sometimes over-stretching, such as the Achilles stretch with the knee bent, can irritate the tendon and cause a bursitis. Prescription foot orthoses can help reduce the torque of the Achilles tendon in these types of cases. Often, the Achilles tendon calcifies near its attachment due to constant torque and tension. Repetitive stress can cause this calcific spur to crack, creating a chronic inflammatory situation that can require surgery. All of these types of chronic Achilles tendinosis that require surgery are successfully treated in over 90 percent of the cases. As with most foot surgery, complete recovery can take up to a year. Though heel pain is common and can be chronic, it does not have to be your weakness (as was the case with the warrior Achilles from Greek mythology). Surgical Treatment At most 95% of heel pain can be treated without surgery. A very low percentage of people really need to have surgery on the heel. It is a biomechanical problem and it?s very imperative that you not only get evaluated, but receive care immediately. Having heel pain is like having a problem with your eyes; as you would get glasses to correct your eyes, you should look into orthotics to correct your foot. Orthotics are sort of like glasses for the feet. They correct and realign the foot to put them into neutral or normal position to really prevent heel pain, and many other foot issues. Whether it be bunions, hammertoes, neuromas, or even ankle instability, a custom orthotic is something worth considering. Where is a heel spur located? Prevention  It is not always possible to prevent heel pain, but there are measures you can take to help avoid further episodes. Being overweight can place excess pressure and strain on your feet, particularly on your heels. This increases the risk of damaging your feet and heels. If you are overweight, losing weight and maintaining a healthy weight by combining regular exercise with a healthy, balanced diet can be beneficial for your feet. You can calculate your body mass index (BMI) to find out whether you are a healthy weight for your height and build. To work out your BMI, divide your weight in kilograms by your height in metres squared. A BMI of less than 18.5 means that you are underweight, 18.5-24.9 means that your weight is healthy, 25-29 means that you are overweight, 30-40 means that you are obese, over 40 means that you are morbidly obese. You can also use the BMI healthy weight calculator to work out your BMI. Overview
Surgical lengthening of the shorter extremity (upper or lower) is another treatment option. The bone is lengthened by surgically applying an external fixator to the extremity in the operating room. The external fixator, a scaffold-like frame, is connected to the bone with wires, pins or both. A small crack is made in the bone and tension is created by the frame when it is "distracted" by the patient or family member who turns an affixed dial several times daily. The lengthening process begins approximately five to ten days after surgery. The bone may lengthen one millimeter per day, or approximately one inch per month. Lengthening may be slower in adults overall and in a bone that has been previously injured or undergone prior surgery. Bones in patients with potential blood vessel abnormalities (i.e., cigarette smokers) may also lengthen more slowly. The external fixator is worn until the bone is strong enough to support the patient safely, approximately three months per inch of lengthening. This may vary, however, due to factors such as age, health, smoking, participation in rehabilitation, etc. Risks of this procedure include infection at the site of wires and pins, stiffness of the adjacent joints and slight over or under correction of the bone?s length. Lengthening requires regular follow up visits to the physician?s office, meticulous hygiene of the pins and wires, diligent adjustment of the frame several times daily and rehabilitation as prescribed by your physician.  Causes The causes of LLD may be divided into those that shorten a limb versus those that lengthen a limb, or they may be classified as affecting the length versus the rate of growth in a limb. For example, a fracture that heals poorly may shorten a leg slightly, but does not affect its growth rate. Radiation, on the other hand, can affect a leg's long-term ability to expand, but does not acutely affect its length. Causes that shorten the leg are more common than those that lengthen it and include congenital growth deficiencies (seen in hemiatrophy and skeletal dysplasias ), infections that infiltrate the epiphysis (e.g. osteomyelitis ), tumors, fractures that occur through the growth plate or have overriding ends, Legg-Calve-Perthes disease, slipped capital femoral epiphysis (SCFE), and radiation. Lengthening can result from unique conditions, such as hemihypertrophy , in which one or more structures on one side of the body become larger than the other side, vascular malformations or tumors (such as hemangioma ), which cause blood flow on one side to exceed that of the other, Wilm's tumor (of the kidney), septic arthritis, healed fractures, or orthopaedic surgery. Leg length discrepancy may arise from a problem in almost any portion of the femur or tibia. For example, fractures can occur at virtually all levels of the two bones. Fractures or other problems of the fibula do not lead to LLD, as long as the more central, weight-bearing tibia is unaffected. Because many cases of LLD are due to decreased rate of growth, the femoral or tibial epiphyses are commonly affected regions. Symptoms Back pain along with pain in the foot, knee, leg and hip on one side of the body are the main complaints. There may also be limping or head bop down on the short side or uneven arm swinging. The knee bend, hip or shoulder may be down on one side, and there may be uneven wear to the soles of shoes (usually more on the longer side). Diagnosis There are several orthopedic tests that are used, but they are rudimentary and have some degree of error. Even using a tape measure with specific anatomic landmarks has its errors. Most leg length differences can be seen with a well trained eye, but I always recommend what is called a scanagram, or a x-ray bone length study (see picture above). This test will give a precise measurement in millimeters of the length difference. Non Surgical Treatment Whether or not treatment should be pursued depends on the amount of discrepancy. In general, no treatment (other than a heel life, if desired) should be considered for discrepancies under two centimeters. If the discrepancy measures between two and five centimeters, one might consider a procedure to equalize leg length. Usually, this would involve closure of the growth plate on the long side, thereby allowing the short side to catch up; shortening the long leg; or possibly lengthening the short leg.  how to increase height after 18 in 1 month Surgical Treatment The type of surgery depends on the type of problem. Outpatient procedures may be used to alter the growth of the limb. This is often done through small incisions. If an outpatient procedure is done, your child can continue with most regular activities. Other times, surgery may be very involved and require the use of an external device that is attached to the limb with pins and wires. This device may be left on for months to correct the deformity or lengthen the leg. If this type of surgery is required, your child will be making weekly visits to Cincinnati Children's. Overview
Have you ever been told or noticed that one of your legs is a bit longer than the other? Do you have incidences of lower back pain? These two things could be related. Most individuals have a small difference in their leg lengths. For some, the discrepancy is small and negligible and will not be a contributor to lower back pain. This is usually the case for people if their leg length is less than 5 millimeters. However, a difference of leg lengths greater than 5 millimeters (1/4 inch) can contribute to lower back pain. If you have a leg length difference of greater than 9 mm, then you have a 6X greater likelihood of having an episode of lower back pain. 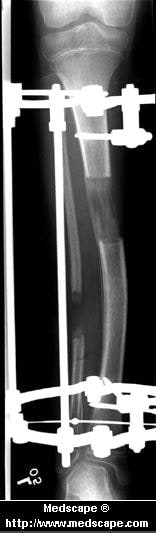 Causes A number of causes may lead to leg length discrepancy in children. Differences in leg length frequently follow fractures in the lower extremities in children due to over or under stimulation of the growth plates in the broken leg. Leg length discrepancy may also be caused by a congenital abnormality associated with a condition called hemihypertrophy. Or it may result from neuromuscular diseases such as polio and cerebral palsy. Many times, no cause can be identified. A small leg length discrepancy of a quarter of an inch or less is quite common in the general population and of no clinical significance. Larger leg length discrepancies become more significant. The long-term consequences of a short leg may include knee pain, back pain, and abnormal gait or limp. Symptoms If your child has one leg that is longer than the other, you may notice that he or she bends one leg. Stands on the toes of the shorter leg. Limps. The shorter leg has to be pushed upward, leading to an exaggerated up and down motion during walking. Tires easily. It takes more energy to walk with a discrepancy. Diagnosis Limb length discrepancy can be measured by a physician during a physical examination and through X-rays. Usually, the physician measures the level of the hips when the child is standing barefoot. A series of measured wooden blocks may be placed under the short leg until the hips are level. If the physician believes a more precise measurement is needed, he or she may use X-rays. In growing children, a physician may repeat the physical examination and X-rays every six months to a year to see if the limb length discrepancy has increased or remained unchanged. A limb length discrepancy may be detected on a screening examination for curvature of the spine (scoliosis). But limb length discrepancy does not cause scoliosis. Non Surgical Treatment Treatment of leg length inequality involves many different approaches, such as orthotics, epiphysiodesis, shortening, and lengthening, which can be used alone or combined in an effort to achieve equalization of leg lengths. Leg length inequality of 2 cm or less is usually not a functional problem. Often, leg length can be equalized with a shoe lift, which usually corrects about two thirds of the leg length inequality. Up to 1 cm can be inserted in the shoe. For larger leg length inequalities, the shoe must be built up. This needs to be done for every shoe worn, thus limiting the type of shoe that the patient can wear. Leg length inequalities beyond 5 cm are difficult to treat with a shoe lift. The shoe looks unsightly, and often the patient complains of instability with such a large lift. A foot-in-foot prosthesis can be used for larger leg length inequalities. This is often done as a temporizing measure for young children with significant leg length inequalities. The prosthesis is bulky, and a fixed equinus contracture may result.  what happens if one leg is shorter than the other? Surgical Treatment The bone is lengthened by surgically applying an external fixation device to the leg. The external fixator, a scaffold-like frame, is connected to the bone with wires, pins, or both. A small crack is made in the bone and the frame creates tension when the patient or family member turns its dial. This is done several times each day. The lengthening process begins approximately five to 10 days after surgery. The bone may lengthen 1 millimeter per day, or approximately 1 inch per month. Lengthening may be slower in a bone that was previously injured. It may also be slower if the leg was operated on before. Bones in patients with potential blood vessel abnormalities, such as cigarette smokers, may also need to be lengthened more slowly. The external fixator is worn until the bone is strong enough to support the patient safely. This usually takes about three months for each inch. Factors such as age, health, smoking and participation in rehabilitation can affect the amount of time needed. Overview
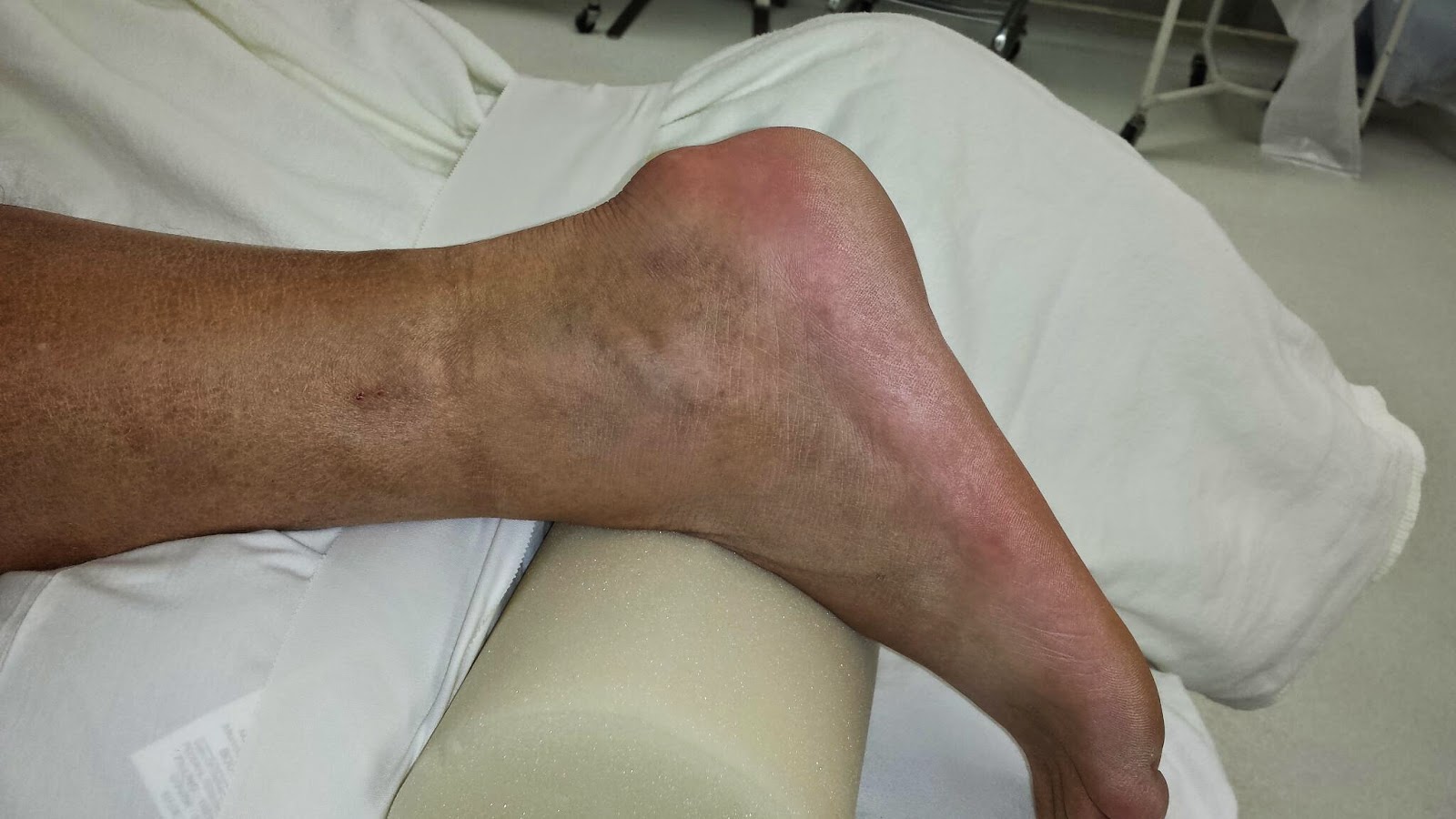 A neuroma is an often painful enlargement of one of your body?s nerves. Morton?s neuroma is the name used to describe nerve enlargement in your foot, particularly enlargement of one of the nerves traveling to your toes in your forefoot. Morton?s neuromas most commonly develop in one of your intermetatarsal nerves, one of many nerve branches within your foot that originated in your spine. Morton?s neuroma is more likely to affect women than men. A neuroma is an often painful enlargement of one of your body?s nerves. Morton?s neuroma is the name used to describe nerve enlargement in your foot, particularly enlargement of one of the nerves traveling to your toes in your forefoot. Morton?s neuromas most commonly develop in one of your intermetatarsal nerves, one of many nerve branches within your foot that originated in your spine. Morton?s neuroma is more likely to affect women than men.Causes The exact cause of Morton?s neuroma is not known, but the choice of footwear seems be a factor. Wearing high heels (shoes with heels over 2 inches) can put extra pressure on the balls of the feet. Wearing tight or pointed toed shoes may squeeze the toes together or otherwise constrict their movement. For that reason, women are about 8 to 10 times more likely to develop Morton?s neuroma compared with men. People who are born with flat feet, high arches, or an abnormal position of the toes are more prone to developing Morton?s neuroma. This may be due to instability around the toe joints. Certain conditions that develop over time, such as bunions or hammer toes, are also associated with Morton?s neuroma. Some sports that involve running, including tennis and other racquet sports, can also increase the chance of developing Morton?s neuroma due to trauma or injury to the foot. Symptoms The primary symptoms include sharp, shooting pain, numbness or paresthesia in the forefoot and extending distally into the toes, typically in the region of the third and fourth toes. Symptoms are aggravated with narrow toe box shoes or those with high heels. There is usually a reduction of symptoms when walking barefoot or wearing shoes with an appropriately wide toe box. Symptoms are also aggravated with shoes that are tied too tight. Diagnosis You might first seek advice from your family doctor about your foot pain. He or she may refer you to a doctor or surgeon who specializes in foot disorders. Before your appointment, you may want to write a list of answers to the following questions. When did your symptoms begin? Did your symptoms begin gradually or suddenly? What type of footwear do you wear for work? Do you participate in sports? If so, what types in particular? What medications and supplements do you take regularly? Your doctor may ask some of the following questions. Is the pain worse in certain pairs of shoes? Does any type of activity ease the pain or worsen it? Are you having pain in any other part of your body? Non Surgical Treatment It can be helpful to perform deep stripping massage techniques along the length of the tibial nerve and the medial and lateral plantar nerves. After properly mobilizing these tissues, moving the foot and toes through a full range of motion to make sure the nerve can move freely will also be helpful. Foot pain like that occurring in Morton's neuroma, can become a debilitating and painful condition. And while massage can be helpful for this condition, it is also clear that improperly applied massage can aggravate it and make it worse. Consequently it is crucial that we use good clinical reasoning and appropriate evaluation methods to most effectively help these clients.  Surgical Treatment Operative treatment of Morton?s neuroma should be entertained only after failure of non-operative management. Standard operative treatment involves identifying the nerve and cutting (resecting) it proximal to the point where it is irritated/injured. This is usually done through an incision on the top (dorsal) aspect of the foot, although an incision on the sole (plantar) aspect of the foot can be used. Some physicians will attempt to treat Morton?s neuroma by releasing the intermetatarsal ligament, and freeing the nerve of local scar tissue. This may also be beneficial. Prevention The best way to prevent a neuroma is by avoiding the things that cause them. Review your risk factors. If relatives have had similar problems, or if you know that you pronate or have any problem with the mechanics of your foot, talk with a podiatric physician about the correct types of shoes and/or orthoses for you. If you are not sure whether you have such a problem, the podiatric professional can analyze your foot, your stride and the wear pattern of your shoes, and give you an honest evaluation. Remember, though, that sometimes neuromas, like other conditions, can develop for no discernible reason. With this in mind, be good to your feet, and be aware of any changes or problems. Don?t wait to report them. There are actually two different types of leg length discrepancies, congenital and acquired. Congenital means that you are born with it. One leg is structurally shorter in comparison to the other. Through developmental stages of aging, the brain senses the step pattern and recognizes some variance. The entire body usually adapts by tilting one shoulder to the "short" side. A difference of under a quarter inch is not very uncommon, demand Shoe Lifts to compensate and usually doesn't have a profound effect over a lifetime.
 Leg length inequality goes largely undiagnosed on a daily basis, yet this condition is very easily remedied, and can eradicate numerous cases of back ache. Treatment for leg length inequality commonly consists of Shoe Lifts. These are generally cost-effective, ordinarily costing under twenty dollars, compared to a custom orthotic of $200 or more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position. Mid back pain is easily the most common ailment impacting people today. Over 80 million people are affected by back pain at some stage in their life. It is a problem which costs companies vast amounts of money every year because of time lost and production. Fresh and improved treatment methods are constantly sought after in the hope of decreasing the economical impact this condition causes.  Men and women from all corners of the earth experience foot ache as a result of leg length discrepancy. In a lot of these situations Shoe Lifts might be of beneficial. The lifts are capable of easing any discomfort and pain in the feet. Shoe Lifts are recommended by countless specialist orthopaedic practitioners". So as to support the human body in a balanced fashion, feet have got a critical task to play. Despite that, it is sometimes the most overlooked zone of the body. Many people have flat-feet which means there may be unequal force exerted on the feet. This causes other body parts like knees, ankles and backs to be affected too. Shoe Lifts ensure that appropriate posture and balance are restored.  Overview OverviewHammer, claw, and mallet toes are toes that do not have the right shape. They may look odd or may hurt, or both. Tight shoes are the most common cause of these toe problems. A Hammer toes is a toe that bends down toward the floor at the middle toe joint. It usually happens in the second toe. This causes the middle toe joint to rise up. Hammer toes often occur with bunions. Claw toe often happens in the four smaller toes at the same time. The toes bend up at the joints where the toes and the foot meet. They bend down at both the middle joints and at the joints nearest the tip of the toes. This causes the toes to curl down toward the floor. A mallet toe often happens to the second toe, but it may happen in the other toes as well. The toe bends down at the joint closest to the tip of the toe. Causes It is possible to be born with a hammer toe, however many people develop the deformity later in life. Common causes include tightened tendons that cause the toe to curl downward. Nerve injuries or problems with the spinal cord. Stubbing, jamming or breaking a toe. Having a stroke. Being a diabetic. Having a second toe that is longer than the big toe. Wearing high heels or tight shoes that crowd the toes and don?t allow them to lie flat. Aging.  Symptoms SymptomsAt first, a hammertoe or mallet toe may maintain its flexibility and lie flat when you're not wearing crowded footwear. But eventually, the tendons of the toe may contract and tighten, causing your toe to become permanently stiff. Your shoes can rub against the raised portion of the toe or toes, causing painful corns or calluses. Diagnosis The earlier a hammertoe is diagnosed, the better the prognosis and treatment options. Your doctor will be able to diagnose your hammertoe with a simple examination of the foot and your footwear. He or Hammer toe she may take an x-ray to check the severity of the condition. You may also be asked about your symptoms, your normal daily activities, and your medical and family history. Non Surgical Treatment In the earlier stages of hammer toe, when the toes can still be manually straightened, then conservative treatment is appropriate. This means wearing shoes which are a half size bigger than normal and which are not narrow around the toes. Exercises to stretch the toes out and strengthen the muscles under the foot which balances the tightness of the top tendons are important. Padding or corn plasters can be used to ease the discomfort of any associated corns and calluses. Surgical Treatment There are generally two methods surgeons use to correct hammer toes, they are joint resection (arthroplasty) or bone mending (fusion), and the location where this is performed on the toe depends on where the toe is buckled. Its important to recognize that most of the surgical work involved the joints of the toe, not the joint of the ball of the foot. Sometimes a toe relocation procedure is needed when the joint of the ball of the foot is malaligned (subluxed or dislocated). 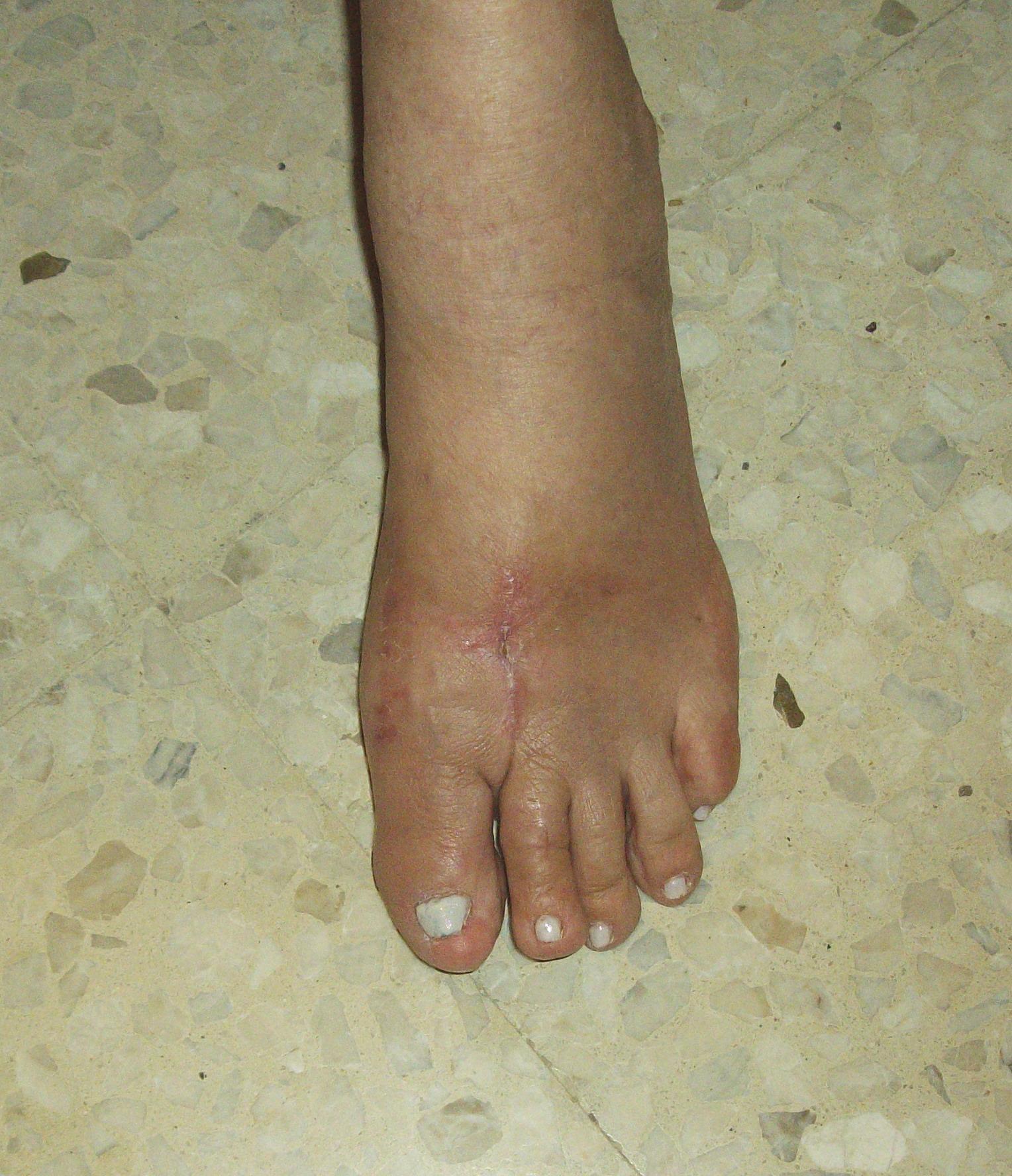 Prevention PreventionWhat to do after you wear your high heels to avoid getting the hammertoes has to do with stretching and opening up the front of the foot. There?s a great product called Yoga Toes that you can slide on your foot and it will stretch and open up all of the toes, elongating and stretching the muscles in the front of the foot. I also advise people to stretch the back of their legs, which is the calf muscle, which puts much less pressure on the front of the foot. The less pressure you have on the front of the foot, the less the foot will contract in and start creating the hammertoes.
Overview
 A bunion is an enlargement of ?the metatarsophalangeal (MTP) joint?, this is the big toe?s base joint that forms when the bone or tissue moves out of place. This forces the toe to bend toward the others, causing an often painful lump of bone on the foot. The MTP joint, which carries lots of weight, is stiff and sore, making even the wearing of shoes difficult or impossible. It also causes swelling of the feet to occur. Hammer toes are also associated with the formation of bunions. A bunion is an enlargement of ?the metatarsophalangeal (MTP) joint?, this is the big toe?s base joint that forms when the bone or tissue moves out of place. This forces the toe to bend toward the others, causing an often painful lump of bone on the foot. The MTP joint, which carries lots of weight, is stiff and sore, making even the wearing of shoes difficult or impossible. It also causes swelling of the feet to occur. Hammer toes are also associated with the formation of bunions.Causes Various factors, including a tight gastrocnemius (or calf) muscle and instability of the arch, contribute to formation of bunions. The tight calf muscle is often hereditary and can cause a bunion because it forces more loading, or pressure, on the forefoot. Ultimately, this can contribute to instability in the bones, ligaments and tendons that form the arch. When it?s unstable, the arch starts collapsing and the metatarsal can shift. Arch instability can also be brought on by obesity, again, due to chronic overloading of the foot. But, by far, the most common contributing factor is childbirth. Bunions are most common in women who have had children. This happens because the hormones that affect their pelvis during childbirth also affect their feet. The hormone is called relaxin, and it allows bones to move and spread. Over time, it can cause the structure of a woman?s feet to gradually stretch and the metatarsal to shift. Symptoms Your bunion may not cause any symptoms. Or you may have pain in your big toe, red or irritated skin over the bunion, and swelling at the base of the big toe. The big toe may point toward the other toes and cause problems in other toes, such as hammer toe . A bunionette can cause similar symptoms at the base of the little toe. Diagnosis The doctor considers a bunion as a possible diagnosis when noting the symptoms described above. The anatomy of the foot, including joint and foot function, is assessed during the examination. Radiographs (X-ray films) of the foot can be helpful to determine the integrity of the joints of the foot and to screen for underlying conditions, such as arthritis or gout. X-ray films are an excellent method of calculating the alignment of the toes when taken in a standing position. Non Surgical Treatment Bunions may be treated with proper shoes and corrective inserts such as toe spacers, bunion or toe separators, as well as bunion cushions and splints. In extreme cases, surgery may be needed to remove the bony enlargement of the first metatarsal bone, realigning the bone, or straightening the big toe. 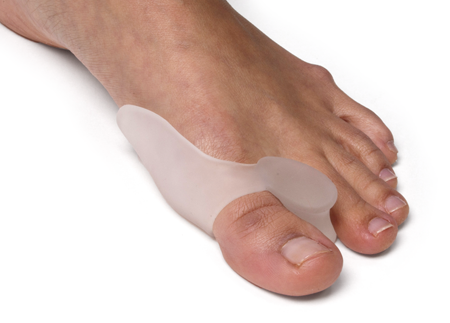 Surgical Treatment Surgery might be recommended if non-surgical treatments fail to provide relief, and you are having trouble walking or are in extreme pain. Surgery can be used to return the big toe to its correct anatomical position. During surgery, bones, ligaments, tendons, and nerves are put back into correct order, and the bump is removed. Many bunion correction procedures can be done on a same-day basis. The type of procedure will depend on your physical health, the extent of the foot deformity, your age, and your activity level. The recovery time will depend on which procedure or procedures are performed. Surgery may be recommended to correct a tailor?s bunion, but is unlikely to be recommended for an adolescent bunion.
Overview
 The Achilles tendon affects your ability to do everything from walking to playing competitive sports. When a patient overstretches his or her Achilles tendon, it can result in a full or partial tear in the tendon, also known as a rupture. In addition to causing a great deal of pain, ruptures can have a profoundly negative impact on your quality of life and prevent you from performing activities you once enjoyed. Because these injuries tend to worsen with time, it?s important to contact a board certified orthopedic surgeon for immediate attention after an Achilles tendon tear. The Achilles tendon affects your ability to do everything from walking to playing competitive sports. When a patient overstretches his or her Achilles tendon, it can result in a full or partial tear in the tendon, also known as a rupture. In addition to causing a great deal of pain, ruptures can have a profoundly negative impact on your quality of life and prevent you from performing activities you once enjoyed. Because these injuries tend to worsen with time, it?s important to contact a board certified orthopedic surgeon for immediate attention after an Achilles tendon tear.Causes The exact cause of Achilles tendon ruptures is hard to say. It can happen suddenly, without warning, or following an Achilles tendonitis . It seems that weak calf muscles may contribute to problems. If the muscles are weak and become fatigued, they may tighten and shorten. Overuse can also be a problem by leading to muscle fatigue . The more fatigued the calf muscles are, the shorter and tighter they will become. This tightness can increase the stress on the Achilles tendon and result in a rupture. Additionally, an imbalance of strength of the anterior lower leg muscles and the posterior lower leg muscles may also put an athlete at risk for an injury to the Achilles tendon. An Achilles tendon rupture is more likely when the force on the tendon is greater than the strength of the tendon. If the foot is dorsiflexed while the lower leg moves forward and the calf muscles contract, a rupture may occur. Most ruptures happen during a forceful stretch of the tendon while the calf muscles contract. Other factors that may increase the risk of Achilles tendon rupture include. Tight calf muscles and/or Achilles tendon. Change in running surface eg: from grass to concrete. Incorrect or poor footwear. A change of footwear eg: from heeled to flat shoes. It is thought that some medical conditions, such as gout, tuberculosis and systemic lupus erythematosus, may increase the risk of Achilles tendon rupture. Symptoms Symptoms of an Achilles tendon rupture usually directly follow a traumatic event where the foot is forced in an upward position at the ankle, causing a sudden tight stretch of the Achilles tendon. There can also be a direct blow to the tendon causing a rupture. There is typically a popping feeling or even a popping sound described during the occurance of the rupture. Typically there is pain with swelling in the region. Often the patient is unable to put weight on this foot as there is too much pain. Diagnosis Your doctor diagnoses the rupture based on symptoms, history of the injury and physical examination. Your doctor will gently squeeze the calf muscles, if the Achilles tendon is intact, there will be flexion movement of the foot, if it is ruptured, there will be no movement observed. Non Surgical Treatment Non-surgical treatment typically involves wearing a brace or cast for the first six weeks following the injury to allow time for the ends of the torn tendon to reattach on their own. Over-the-counter medications, such as ibuprofen or aspirin, may be taken during this time to reduce pain and swelling. Once the tendon has reattached, physical therapy will be needed to strengthen the muscles and tendon. A full recovery is usually made within four to six months.  Surgical Treatment Immediate surgical repair of the tendon is indicated in complete tears. Delaying surgery can lead to shortening of the tendon, formation of scar tissue and decreased blood flow, which can lead to a poor outcome. Following surgery your ankle will be put in an immobilizing device and you will be instructed to use crutches to limit weight bearing and protect the joint. Over the next 2-4 weeks weight bearing will be increased and physical therapy will be initiated. The surgeon will determine the physical therapy timeline and program. Physical Therapy, Treatment will emphasize gradual weaning off the immobilizing device, increased weight bearing, restoration of ankle range of motion and strengthening of the lower leg muscles. It is important that the physician and therapist communicate during the early stages and progress your program based on the principles of healing so as not to compromise the Achilles tendon. Patient will be progressed to more functional activities as normal ankle range of motion and strength is restored. |
|
